Diagnosis of Axial Spondyloarthritis – Interview with Joachim Sieper (Part 1)
Joachim Sieper is professor emeritus of rheumatology at the Benjamin Franklin Campus of the Charité Berlin. In an interview with online editor Eva Reidemeister, he reveals why the term “Bechterew’s disease” is outdated and why we speak of axial spondyloarthritis today.
Eva Reidemeister – freelance editor | Joachim Sieper – rheumatologist
Also: For the diagnosis, the medical specialists from radiology and rheumatology have to work closely together. Read on to learn how.
Eva Reidemeister: It may be because of my background as an editor, but the first thing that struck me when I started researching the topic was that axial spondyloarthritis has undergone a conceptual change. People used to talk about Bechterew’s disease. This is now considered outdated and other terms are commonly used to describe the disease. What are they — and why?
Joachim Sieper: The old nomenclature goes back to around 1900. At that time, the diagnosis could be made if the spine was completely ossified and completely stiff. And the term Morbus Bechterew comes from this time.
Bechterew (also “Bekhterev”) was a Russian neurologist who lived at the end of the 19th century. There is also the term ankylosing spondylitis, which means: The spine is ossified. These terms come from that time.
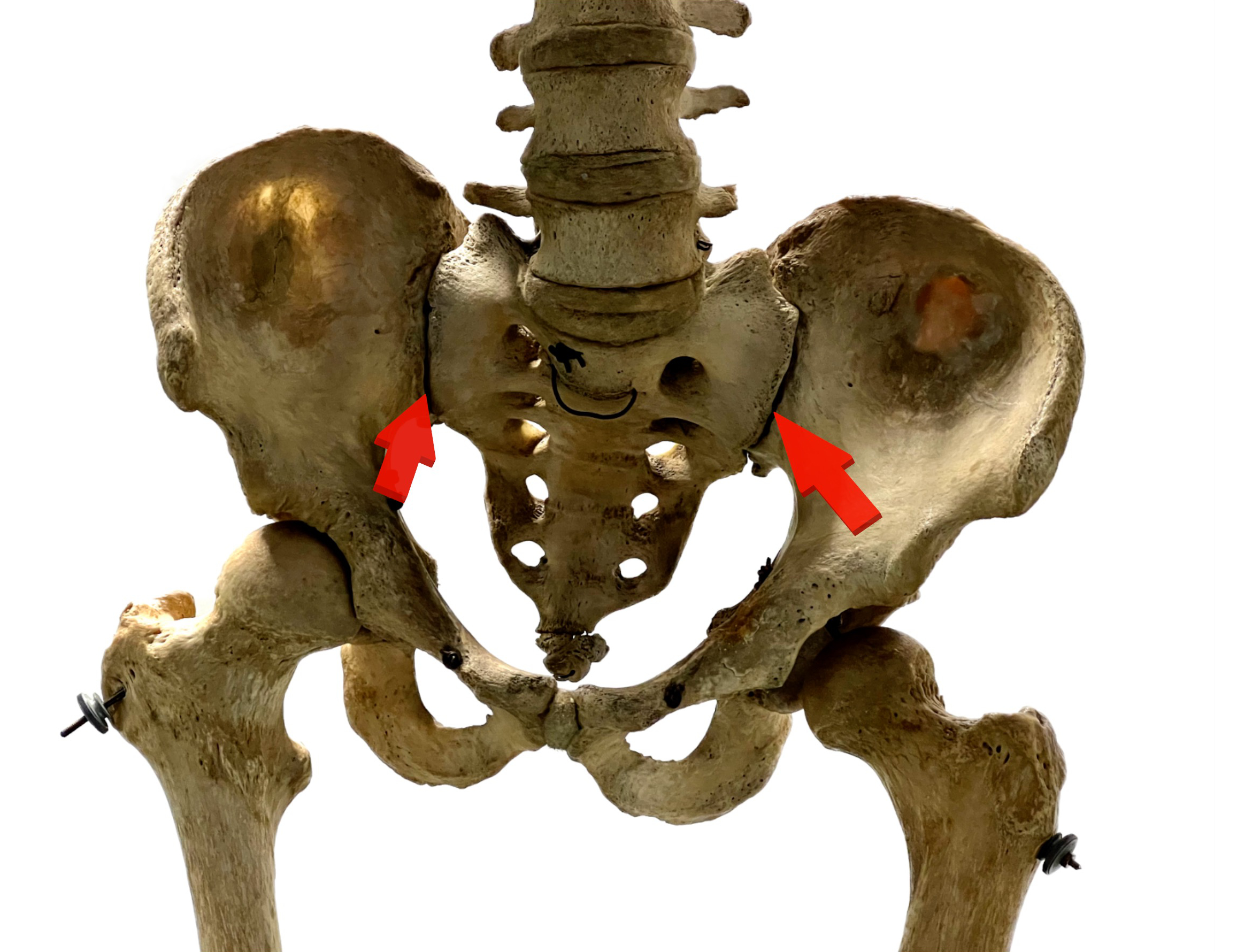
However, it has been known since the 1930s that the disease starts in the sacroiliac joints, before the spine is affected, and that is why the pelvis has been X-rayed and the changes in the pelvic X-ray have played a decisive role in diagnosis. Since about the 1990s, there has been a growing realization that what you see on X-rays is a result of the inflammation that preceded it.
Human pelvis. Arrows point at sacroiliac joints.
X-rays only show something if the bone is destroyed or if increased new bone formation takes place as a reaction to the bone destruction. Accordingly, you only see something relatively late. This is where magnetic resonance imaging (MRI) comes into play. Scintigraphy used to be deployed, but it is relatively unspecific and therefore less significant in diagnosing. MRI, on the other hand, offers the enormous advantage that you can see the inflammation in the bones.
So you don’t have to wait until the bone is destroyed. This makes early diagnosis possible. That’s why we now say axial spondyloarthritis. This includes the entire disease group, regardless of whether there are X-ray changes or not. This can be broken down further into:
- Non-radiographic axial spondyloarthritis (nr-axSpA) with no radiographic changes visible
- Radiographic axial spondyloarthritis with evidence of radiographic changes in the sacroiliac joints
In addition, the term ankylosing spondylitis exists.
ER: This means that the change in terminology has a lot to do with how the disease has been diagnosed in the past and today. After all, how common is the diagnosis of axSpA today — and how is it made?
JS: There is an older study from a general practice in England. We always refer to that. It’s still a bit vague, but we estimate that about 5 % of people with chronic back pain who go to the doctor because of it have axSpA. That’s relatively little. And because of this, any test that is positive on its own results in a relatively low post-test probability.
This is a term that is discussed again and again in connection with the coronavirus: What is the probability that I have the disease if I have antibodies? But that’s generally true in medicine, and because we have a relatively low pre-test probability, you cannot diagnose with a simple test. You have to make various tests and take the overall picture into account.
With this in mind, we have been saying for a number of years that there are two strategies. For once, what do you offer the doctor who first sees this patient with chronic back pain? We actually don’t think they are able to diagnose well just like that — because it’s complex, and one needs experience. And that’s why we have developed other so-called screening parameters, i.e. “red flags”, that show the doctors when they should also think about axSpA when a patient with symptoms is sitting in front of them.
ER: Back pain is actually a widespread disease, but axSpA is rare. So how do you get a grip on axial spondyloarthritis in the first place? Initially, I would present a problem that isn’t very specific at the doctor’s office. I would probably complain of lower back pain. But that can be caused by many things, for example by stress.
JS: But if, for example, this patient says, “Oh, the back pain comes on in the morning when I wake up and if I walk around a bit, it gets better. But when I sit down, it doesn’t get any better.” Then that’s an indication that axial spondyloarthritis may be an issue there.
But also when other parameters are positive, for example psoriasis is present or a laboratory test was carried out and this gene, HLA-B27, was positive, this should lead one to investigate further.
Especially in young patients, if only one of these parameters is positive, we have recommended referral to a rheumatologist. In some countries, specialists in physical medicine also take care of these patients. In Germany, this is most likely an assignment in the field of rheumatology, and the rheumatologist then has to do all the examinations.
ER: What questions would one ask in the anamnesis, for example? I am also thinking of secondary diseases such as psoriasis, which often occur together with axSpA. So how would you go about doing that?
JS: When taking the medical history, one must ask when the pain occurs (rather in the morning or more in the evening). How does it feel when active or moving? In addition, they are asked about psoriasis, Crohn’s disease and other diseases — including whether they may have run in the family. Then the HLA-B27 gene and inflammation parameters such as blood sedimentation and C-reactive protein must be determined. And then imaging comes into play.
Lower back pain.
The rheumatologist usually seeks a dialogue with the radiologist. The reason: We cannot see back pain. Therefore, we urgently need a method to help us interpret the cause of this pain, and imaging helps both in the early phase, to detect the inflammation, and in the advanced phase, when the inflammation is already causing bone destruction and new bone formation in the spine and pelvis.
ER: From a rheumatological perspective, what is the greatest challenge in diagnosing axSpA?
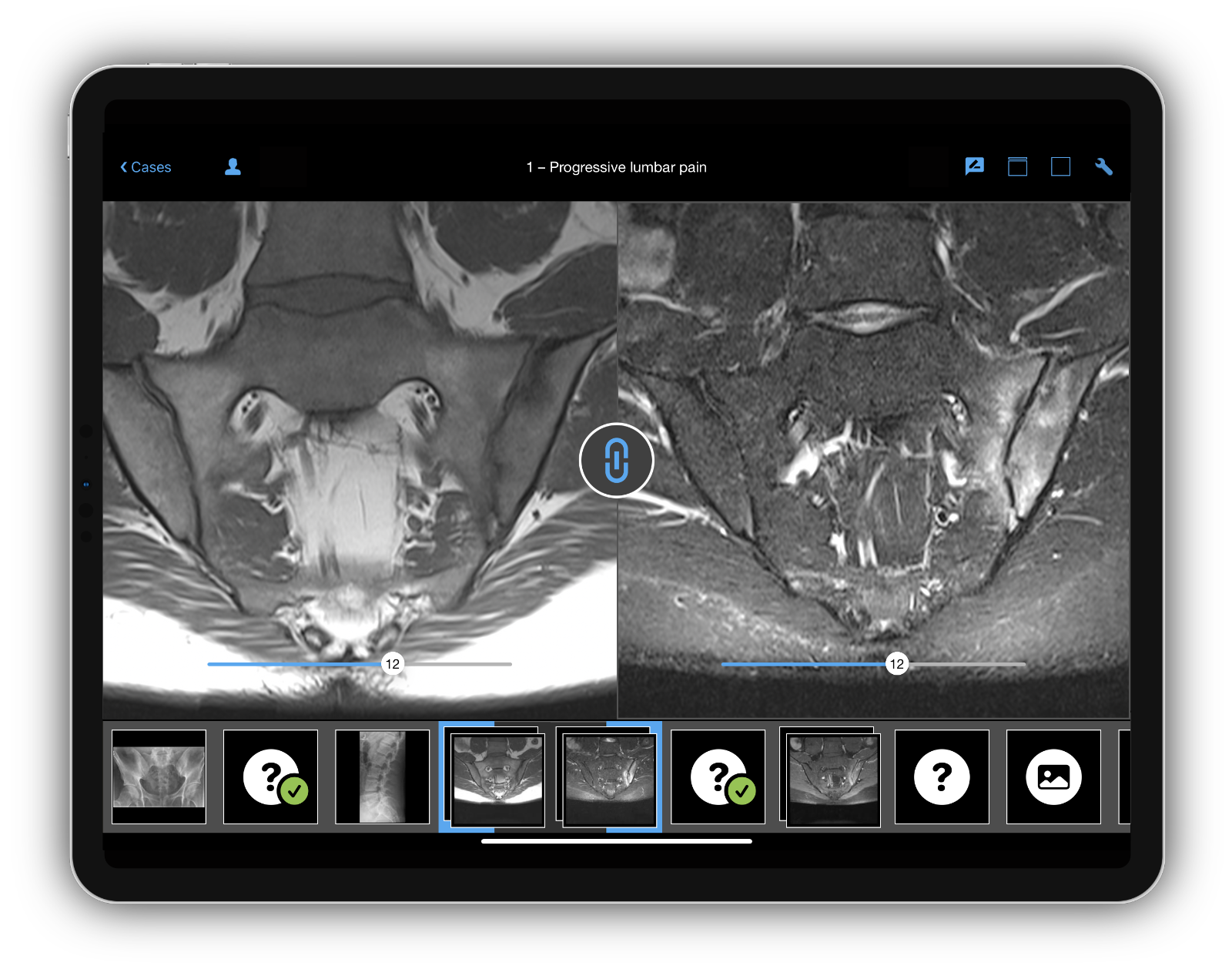
JS: First of all to summarize all clinical laboratory and imaging parameters and then also to interpret the imaging. Because there is always a relatively large differential diagnosis for positive findings, as is generally the case in medicine. So, using the example of a positive MRI result: You see edema, i.e. an accumulation of water in the bone, and that can be the first sign of axial spondyloarthritis, because the immune process, which is not exactly understood, triggers local inflammation.
MRI of an inflamed sacroiliac joint. Imaging example taken from the BerlinCaseViewer app.
As part of research, this was punctured in patients, i.e. a sample was taken with a needle, and clear inflammatory processes were seen. But in the MRI, for example, mechanical stress looks very similar, for example when jogging or during pregnancy, where the pressure on the pelvis is high. However, this stress is mechanical and not triggered by an immune process. However, this cannot initially be decided on the basis of imaging alone. You need experience, and you have to talk to the radiologist. In addition, all other findings that I have listed and information from the medical history must be included.
So what radiologists have to take into account is that they cannot make a diagnosis solely on the basis of imaging. They can practically only describe what they see, and that then has to be summarized by someone — usually this is a rheumatologist then.
ER: This means that interdisciplinary cooperation is particularly important for this disease — that rheumatology and radiology work closely together.
JS: Yes, exactly.
ER: Rheumatologist know, so to speak, about the inflammatory processes, while radiologists can see what the disease looks like. What can both learn from each other, or what is the takeaway?
JS: As mentioned, it is important for the radiologist not to be able to make a diagnosis based on imaging alone. Symptoms and other parameters (HLA-B27, CRP) must be included, for example: Does the patient also have a swollen knee or heel? Because these are other manifestations of the disease outside of the axial skeleton. And because that is outside the interest of radiologists, they have to seek dialogue with rheumatologists or the rheumatologist will make the diagnosis in the end.
Interdisciplinary discussion of MRI findings.
For the rheumatologist, on the other hand, it is very important to always keep in mind that there is a relatively large differential diagnosis, why an imaging finding can be positive, and that usually, as a rheumatologist, one does not have the experience to interpret this correctly. Also, the other diseases that come into question, for example bone marrow edema during pregnancy — one might not be well versed with these. Then again, you need the advice of the radiologist.
ER: What is currently being done to ensure that these two disciplines work more closely together, also to exchange ideas and to find out from the other side what the current state of research is?
JS: In the field of spondyloarthritis there are 5 to 10 groups worldwide where the cooperation between rheumatologists and radiologists is very intensive. These are then also the groups from which the proposals for definitions, positive findings, differential diagnoses and so on emanate. They also organize training courses, which in the past were mostly for rheumatologists.
It would actually make sense to involve more radiologists in the future. To some extent this is already happening, but not all radiologists devote their work to the axial skeleton – or to rheumatism, for example if the hands are also affected in rheumatoid arthritis.
There is still room for improvement when it comes to working together. That was also an idea behind the BerlinCaseViewer, that with such an app you can also interest a wider circle, including radiologists, who can then use the app to look at the various cases.
ER: Is that how the BerlinCaseViewer came about? After all, Kay G. Hermann as a radiologist and you as a rheumatologist are behind the app.
JS: This cooperation has actually existed for 25 years. We were also one of the first back then, when the Benjamin Franklin University Hospital was not yet part of the Charité, when we started to carry out MRI examinations in patients with spondyloarthritis. That was Doctor Bollow — and Doctor Hermann studied under him and was in the same department. He then continued this collaboration, so that we have actually been working continuously on these issues, which we have now outlined a bit, for 25 years.
There are a number of groups around the world that are also working on this. Just as an example: Mr. Hermann and I have been to Brazil — I think even twice — and have done training courses there on the interpretation of imaging in connection with the clinical presentation of patients. As a rule, however, these events were always attended by rheumatologists, which was mainly due to the local organization, who were in charge of the invitations. So that’s a goal, further improving this interaction.
ER: The BerlinCaseViewer has now also openly adopted other topics, such as the coronavirus, due to the current situation. The app can also be used for other diseases. Is that a plan for the future?
JS: I’m a rheumatologist and I stand for spondyloarthrides — so for me personally, probably not — but it is certainly conceivable to use the energy that was also put into the software development in this way. We put together the case library, played the cases on the iPads and took the iPads with us.
Hands-on workshop with iPads.
We also developed a web version in time for the Corona crisis. And have already taken four online courses. A lot of work has gone into this, and it can be used for other diseases without any problems. It is also conceivable, for example, to expand into the field of neurology, but here Mr. Hermann is clearly the better contact person to explain more details about where the app is headed in the future.
Download BerlinCaseViewer
Related posts:
This post is also available in: German